We’re proud to highlight a new paper citing Pluto published in Cardiovascular Research by Dr. Priyatansh Gurha at The University of Texas Health Science Center.
In conditions like heart failure, myocardial infarction (heart attack), and cardiomyopathy, the heart muscle is damaged or weakened, leading to inefficient heart function. By replacing the lost or damaged cardiomyocytes with new, functional ones derived from pluripotent stem cells, it's possible in the future that we’ll be able to improve heart function and potentially reverse some of the damage caused by these conditions. This approach represents a significant advancement in regenerative medicine, offering hope for more effective treatments for various heart diseases.
"Creating" cardiomyocytes
Human pluripotent stem cell-derived cardiomyocytes (iPSC-CMs) are one of the most widely used cell-based models originating from non-embryonic stem cells1, and they offer researchers a platform for investigating factors that regulate the maturation of cardiomyocytes2. In order to transition from an immature fetal state to adult CM state, the expression of genes involved in myofibril formation, oxidative phosphorylation and other pathways must change in a coordinated fashion. However, the immaturity of the induced PSC-derived CMs currently prevents them from being used functionally, e.g. to replace damaged CMs.
In this paper, Dr. Gurha and his team study an epigenetic enzyme lysine demethylase 5 (KDM5), which is a potential regulator of genes involved in cardiac development and mitochondrial function. By understanding the role of KDM5 in iPSC-CMs, the researchers are helping the field move closer to interventions that can enhance iPSC-CM maturation, thereby enabling their potential use as a therapy
Explore key findings: CUT&RUN analysis in Pluto
To investigate KDM5’s effect, the authors treated iPSC-CMs with a KDM5 inhibitor, KDM5-C70, and measured protein-DNA interactions using the Cleavage Under Targets and Release Using Nuclease (CUT&RUN) assay. After sequencing, the FASTQs were uploaded to Pluto and run through the nf-core/cutandrun pipeline to produce a detailed MultiQC report that is stored for easy reference later. Pluto also automatically generates a dynamic methods section so the Gurha Lab could utilize information in their manuscript without additional effort.
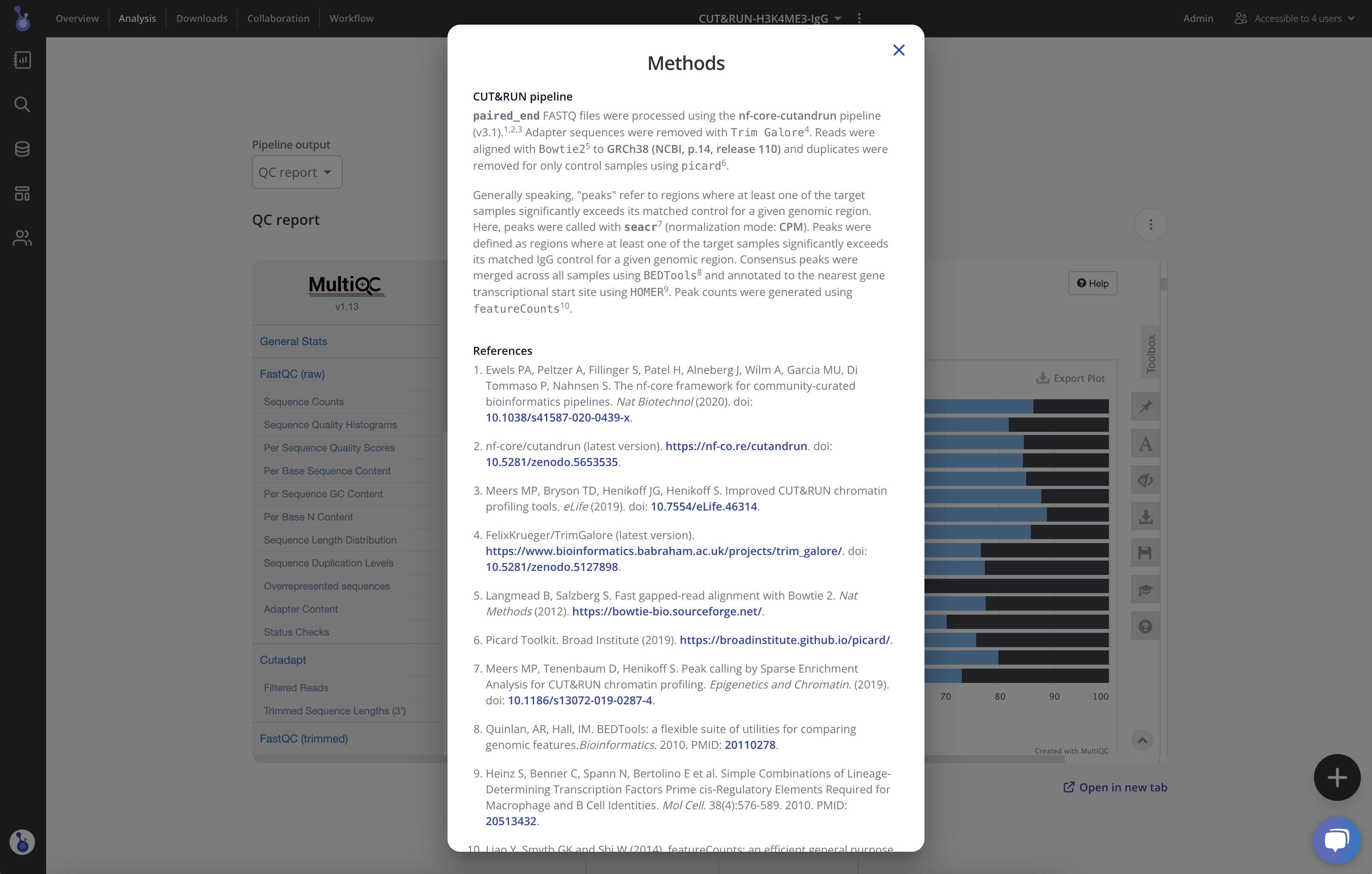
Learn more about CUT&RUN analysis in Pluto
To identify the genome-wide H3K4me3 enriched sites, the authors performed differential binding analysis comparing untreated iPSC-CMs to iPSC-CMs treated with the KDM5-C70 inhibitor. The volcano plot shows peaks that had increased binding with KDM5 inhibition in red, and peaks that had decreased binding in blue.
Note: the plot above shows live data from Pluto for this experiment. Click the button in the upper right corner to view the methods. Learn how to create your own public plot share links with Pluto here.
Pathway analysis (GSEA) using these differentially bound regions showed a coordinated upregulation of genes involved in fatty acid oxidation.
The Pluto team congratulates the Gurha Lab on these novel and impactful findings! Be sure to check out the publication in Cardiovascular Research.
References
1 S.D. Burnett, A.D Blanchette, W.A. Chiu & I Rusyn. Human induced pluripotent stem cell (iPSC)-derived cardiomyocytes as an in vitro model in toxicology: strengths and weaknesses for hazard identification and risk characterization. Expert Opinion on Drug Metabolism & Toxicology. 2021. https://doi.org/10.1080/17425255.2021.1894122
2 M. Deogharia, L. Venegas-Zamora, A. Agrawal, M. Shi, A.K. Jain, K.J. McHugh, F. Altamirano, A.J. Marian, P. Gurha. Histone demethylase KDM5 regulates cardiomyocyte maturation by promoting fatty acid oxidation, oxidative phosphorylation, and myofibrillar organization. Cardiovascular Research. 2024. https://doi.org/10.1093/cvr/cvae014

